Silicon Implants
I opted to have silicon implants (plus I didn’t have the juicy belly bits to construct a new bouncing breast). But there are other options: TRAM flap and Pedicle flap. In my case the procedure went a little something like this:
On February 1st I had a double mastectomy immediate reconstruction. My breast surgeon made a full incision around my nipple taking it away and through the opening removed all the breast tissue. Some breast tissue goes up under the armpit, which mine did, so he travelled up there through the same incision site. This part of the operation took two hours.
Next my plastic surgeon entered the theatre and performed the last stage – the immediate reconstruction. He inserted saline tissue expanders into both breasts through the same open site, and then sewed me up. So I have one long scar across each breast with no nipple. I resemble more of a boy’s chest than a woman’s.
Do you remember the 1980’s blue and white stripped t-shirt with a silver zipper across each breast? The zipper effect is what my chest looks like.
The plastic surgeon inserted drains into the breast mound area through my skin (entering from the side of my torso nearish to my armpit) and sutured them in place – rather an inadequate child’s papier mache octopus. The drains remained in place for one week. They took away fluid and excess blood from the breast area. This part of the operation took two hours. All up, I was under a general anaesthetic for four and bit hours. I woke with a tightly wrapped dressing over my chest.
The anesthetist did a stellar job. She phoned me the Friday before mastectomy Monday and talked through my prior bad reactions, nausea etc and how she was going to handle things. I took two Phenergan (anti-histamine, anti-nausea, anti-awake) pills at 11am, and by 1:30pm when I was due to go into theatre I could barely remain awake. This is a good thing.
When the time came to go in my breast surgeon loomed over me to confirm I knew exactly what was about to happen. He had a blue tinge under each eye as if he’d been working too hard or too late. ‘Okay?’ he asked.
‘I’m in the middle of one of the weirdest days of my life.’
He patted my left shoulder in sympathy, and then I was wheeled into theatre. And. Action.
Two weeks after the procedure my surgeon had a look-see and deemed that he could start inflating me in one week. My chest area was/is hyper-sensitive; a strange removed feeling. Imagine wearing a fat suit over your body after a severe car accident left you bruised and lacerated. A good old friend comes to wish you luck and pats you on your fat suit (because let’s face it, you look funny) right over the area where your ribs connected with the steering wheel. You see him touching the fat suit, but can’t feel the contact. What you feel is the pressure of his finger over the wounded area. The disconnect between sensations is deeply uncomfortable. When my surgeon touched my chest I almost jumped off the examination table.
It’s the 26th February and I haven’t taken pain meds for two weeks.
Last Monday (22nd) the inflating process commenced. The plastic surgeon has a nurse who performs the saline injections into the tissue expander. On the expander is a pin cushion (valve) the size of a fifty cent piece with a magnet in it. The nurse put a divining gadget the size of a mobile phone over my breast mounds to align magnet to magnet. Once found a needle is inserted through the skin and muscle into the valve. If she misses a shooting pain goes up into your armpit. She missed once. However, if she gets it right there’s hardly any pain. Sixty mils get injected into each expander every week until you’re the desired size. They do this to stretch the skin to fit the ‘choose your own adventure’ permanent silicon implants, which are inserted later. Right now I have little raised mounds on my chest. Feels fine.
Next comes replacing the expanders with silicon bags, then nipple and areola reconstruction (all pending – I’ll tell you when I know the deal).
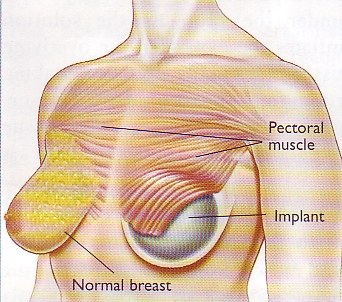
The Australian Society of Plastic Surgeons Inc. 'Breast Reconstruction: A guide for patients,' Edition 1, 15 March 2002.
TRAM (Transverse Rectus Abdominis Myocutaneous) flap or free flap
In this procedure, the breast with cancer is surgically removed, and a portion of the abdomen tissue group, including skin, adipose tissues, minor muscles and connective tissues, is taken from the patient’s abdomen and transplanted onto the breast site (accessed from Wikipedia 26th February, 2010 at 2:57pm).
Some women like this because they get a tummy tuck and boob job all under the same operation. Plus, they’ve just got rid of breast tissue with cancer in it. The major positive of this surgery is that you go into theatre with your original breasts and wake up with new ones that bounce like your former ones. The negative is that it reduces the strength in your abdominal muscles (there’s also quite a bit of scarring).

The Australian Society of Plastic Surgeons Inc. 'Breast Reconstruction: A guide for patients,' Edition 1, 15 March 2002.
Pedicle flap
Tissue used to form the flap is free from the donor site, but the blood supply is not divided. The flap remains attached by the blood vessels and can be moved as far as the blood vessels allow. It is repositioned at the site of the removed breast through the mastectomy incision. After being formed into a breast shape, it is stitched into position (The Australian Society of Plastic Surgeons Inc. ‘Breast Reconstruction: a guide for patients’, edition 1, 2002).
The places they can remove from (donor site) are the back muscles (latissimus dorsi) or just under the breast area (rectus muscle). From talking with women who’ve had a reconstruction using their own tissue all of them have had TRAM flap procedures, not pedicles.

[…] Breast Reconstruction February 2010 5 […]
Really enjoyed this update, is there any way I can receive an update sent in an email every time you publish a fresh update?
Yes, you can ‘follow’ my blog – go to main page and put in your details. Josie x.
Yes, ‘follow’ my blog. Can find on home page. Thank you.